Massage or stretching? Effectiveness in reducing muscle pain in older adults doing strength training
Main Article Content
Abstract
Introduction: globally, the population is aging; it is expected that by 2030, one in six people will be over 60 years old. Delayed Onset Muscle Soreness (DOMS) is a structural pain that frequently appears 24 to 48 hours after unusual or high-intensity exercise. In older adults, DOMS can be more debilitating due to age-related physiological changes, such as decreased muscle elasticity and mass. Although massage therapy and static stretching are proposed as treatments, their specific impact on reducing DOMS in this population is not well documented.
Objective: to compare the effectiveness of relaxation massage therapy and static stretching in reducing the occurrence of delayed onset muscle soreness (DOMS) symptoms in people over 60 years of age after a physical intervention program.
Methodology: we conducteda quasi-experimental, randomized, single-blind study. The sample consisted of 30 individuals over 60 years of age (6 men, 24 women), randomly divided into two groups of 15 participants each: a massage therapy group and a static stretching group. All participants performed a 60-minute resistance training intervention using elastic bands to induce delayed onset muscle soreness (DOMS) in the trapezius muscle. Pain intensity (Numerical Analog Scale - NAS), pressure pain threshold (Algometer), and functional status (Functional Pain Scale - FPS) were assessed. Because the data did not follow a normal distribution, the non-parametric Friedman and Durbin-Conover tests were used for comparisons.
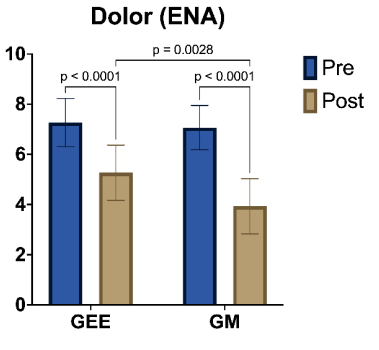
Results: both groups showed a reduction in mean NAS and FPS scores, suggesting an overall improvement. The Friedman test showed significant overall differences (p < .001). Post-hoc comparisons (Durbin-Conover) revealed a statistically significant difference between the groups in the final NAS (p = 0.002), favoring massage therapy. However, no significant differences were found between the groups for the final EFD (p = 0.615) or the final Dolorimeter (p = 0.900).
Discussion: the results suggest that both interventions had a positive impact on reducing DOMS, which is consistent with previous studies. The post-hoc analysis indicated that massage therapy had a more consistent impact on reducing perceived pain (NAS). The lack of significant differences in functional measures (EFD) between the groups suggests that both interventions may have similar effects on this specific variable.
Conclusions: the study demonstrated that both static stretching and relaxation massage therapy are effective strategies for reducing DOMS in older adults. However, the results indicate that massage therapy has a more consistent impact on reducing pain perception and improving muscle function, suggesting that it could be the preferred intervention for a faster recovery.
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License.
Usted es libre de:
- Compartir: copiar y redistribuir el material en cualquier medio o formato para cualquier propósito, incluso comercialmente.
- Adaptar: remezclar, transformar y construir a partir del material para cualquier propósito, incluso comercialmente.
- La licenciante no puede revocar estas libertades en tanto usted siga los términos de la licencia
Bajo los siguientes términos:
- Atribución: Usted debe dar crédito de manera adecuada, brindar un enlace a la licencia, e indicar si se han realizado cambios. Puede hacerlo en cualquier forma razonable, pero no de forma tal que sugiera que usted o su uso tienen el apoyo de la licenciante.
- Compartir igual: — Si remezcla, transforma o crea a partir del material, debe distribuir su contribución bajo la misma licencia del original.
- No hay restricciones adicionales — No puede aplicar términos legales ni medidas tecnológicas que restrinjan legalmente a otras a hacer cualquier uso permitido por la licencia.
References
World Health Organization. Ageing and health. [Internet]. 2022 [cited 2025 Sep 10]. Ginebra:WHO. Disponible en: https://www.who.int/es/news-room/fact-sheets/detail/ageing-and-health
Concha-Cisternas Y, Castro-Piñero J, Vásquez-Muñoz M, Molina-Márquez I, Vásquez-Gómez J, Guzmán-Muñoz E. Effects of neuromuscular training on postural balance and physical performance in older women: randomized controlled trial. J. Funct Morphol. Kinesiol. 2024;9(4):195 [Internet].[cited 2025 Sep 10]. doi: 10.3390/jfmk9040195.
Suputtitada A, Chen CPC, Ngamrungsiri N, Schmitz C. Effects of repeated injection of 1 % lidocaine vs. radial extracorporeal shock wave therapy for treating myofascial trigger points: a randomized controlled trial. [Internet]. Medicina. 2022;58(4):479 [cited 2025 Sep 10. doi: 10.3390/medicina58040479
Bagheri R, Taghizadeh Del khoush C, Mirmohammadkhani M, Safavi Farokhi Z, Bakhshi S. Comparison of dry needling and inhibitory kinesio taping in treatment of myofascial pain syndrome of the upper trapezius muscle: a randomized controlled trial. J Chiropr Med [Internet]. 2022 [cited 2025 Sep 10];21(1):23-31. doi: 10.1016/j.jcm.2022.01.003
Mohamadi M, Piroozi S, Rashidi I, Hosseinifard S. Friction massage versus kinesiotaping for short-term management of latent trigger points in the upper trapezius: a randomized controlled trial. Chiropr Man Therap [Internet]. 2017 [cited 2025 Sep 10];25(1):1–6. doi 10.1186/s12998-017-0156- 9
Suarez-Ramos C, Gonzalez-Suarez C, Gomez IN, Gonzalez MK, Co PH, Llamas JA. Effectiveness of ultrasound guided interfascial hydrodissection with the use of saline anesthetic solution for myofascial pain syndrome of the upper trapezius: a single blind randomized controlled trial. Front Rehabil Sci. 2023;4:1281813. doi: 10.3389/fresc.2023.1281813.
Navarro-Santana MJ, Valera-Calero JA, Romanos-Castillo G, Hernández-González VC, Fernández-de-las-Peñas C, López-de-Uralde-Villanueva I, et al. Immediate effects of dry needling on central pain processing and skin conductance in patients with chronic nonspecific neck pain: a randomized controlled trial. [Internet]. J. Clin. Med. 2022;11(22):6616. [cited 2025 Sep 10]. doi: 10.3390/jcm11226616.
Downie WW, Leatham PA, Rhind VM, Wright V, Branco JA, Anderson JA. Studies with pain rating scales. Ann RheumDis [Internet]. 1978 [cited 2025 Sep 10];37(4):378–81. Disponible en: https://ard.eular.org/action/showFullText?pii=S0003496724144160
Fischer AA. Pressure algometry over normal muscles. Standard values, validity and reproducibility of pressure threshold. Pain [Internet]. 1987 [cited 2025 Sep 10];30(1):115–26. doi: 10.1016/0304-3959(87)90089-3
Guzmán-Muñoz E, Mendez-Rebolledo G, Concha-Cisternas Y, Alarcón-Rivera M, FaúndezCasanova C. Diseños de investigación cuantitativa en ciencias de la actividad física y la salud. Revista Ciencias de la Actividad Física UCM [Internet]. 2025[cited 2025 Sep 10];26(2):63–85. doi: 10.29035/rcaf.26.2.5
Arsovski D. Effectiveness of medical massage in reducing neck pain among multiple occupational groups: a longitudinal study. [Internet]. Int J Ther Massage Bodywork. 2024 [cited 2025 Oct 4];17(3):23. doi: 10.3822/ijtmb.v17i3.993
Narenthiran P, Granville Smith I, Williams FMK. Does the addition of manual therapy to exercise therapy improve pain and disability outcomes in chronic low back pain: A systematic review. J Bodyw Mov Ther [Internet]. 2025 [cited 2025 Sep 10];42:146–52. doi: 10.1016/j.jbmt.2024.12.004
Espinoza Acuña G, Sánchez Ureña B, Rojas Valverde D, Gutiérrez Vargas JC, Cordero Duarte K, Blanco Romero L, et al. Efecto agudo del estiramiento estático y dinámico sobre el rendimiento y la percepción de esfuerzo en ejercicio contrarresistencia. MHSalud [Internet]. 2021[cited 2025 Oct 4];18(1):1–18. doi: 10.15359/mhs.18-1.1
Suresh V, Venkatesan P, Babu K. Effect of proprioceptive neuromuscular facilitation and cranio-cervical flexor training on pain and function in chronic mechanical neck pain: A randomized clinical trial. Physiother Res Int [Internet]. 2024 [cited 2025 Sep 10];29(1):e2058. doi: 10.1002/pri.2058.
Fahrudin P, Ridwan A. Acute Acute Effects of combined massage therapy and sun salutation yoga on pain reduction and range of motion in patients with nonspecific low back pain. J. Welln Compl Trad Med [Internet]. 2025[cited 2025 Sep 10];1(1):37–46. doi: 10.21831/jwctm.v1i1.1125
Sarhan Ahmed N, Shokry Abd Allah E, Mohammed Ahmed F. Effect of intradialytic stretching exercises on elderly patients’ muscle cramps and stress. Cuest. fisioter [Internet]. 2024 [cited 2025 Sep 10];53(02):4070–88. doi: 10.48047/5c8ppz07
Papoli AF, Hosseini SM, Mirkarimpour SH. Effects of different treatments on pain, functional disability, position sense and range of motion in elite bodybuilders with chronic low back pain. SciRep [Internet]. 2024 [cited 2025 Sep 10];14(1):1–10. doi: 10.1038/s41598-024-59684-2
Nereyda Z, Ramos A, Rocío B, Colmenero R, Zarai M, Dávila G, et al. Influencia del masaje ZNAR y la inmersión en agua fría en el proceso inflamatorio, Creatin Kinasa y percepción al dolor muscular en jugadores de voleibol. [Internet]. Retos. 2022(44):95-102. [cited 2025 Oct 5]. Disponible en: https://dialnet.unirioja.es/servlet/articulo?codigo=8104616
Fowler BD, Palombo KTM, Feland JB, Blotter JD. Effects of whole-body vibration on flexibility and stiffness: a literature review. Int J Exerc Sci [Internet]. 2019 [cited 2025 Sep 10];12(3):735. doi: 10.70252/TJVC4921
Ibáñez J, Zicher B, Burdet E, Baker SN, Mehring C, Farina D. Peripheral neural interfaces for reading high-frequency brain signals. Nat Biomed Eng [Internet]. 2025 [cited 2025 Oct 1];9(9):1391–402. doi: 10.1038/s41551-025-01445-1
Choi JM, Cho EY, Lee BH. Effectsof dynamic stretching combined with manual therapy on pain, rom, function, and quality of life of adhesive capsulitis. Healthcare [Internet]. 2023 [cited 2025 Sep 10];12(1):45. doi: 10.3390/healthcare12010045
Wen S, Muñoz J, Mancilla M, Bornhardt T, Riveros A, Iturriaga V, et al. Mecanismos de modulación central del dolor: revisión de la literatura. Int J. Morphol [Internet]. 2020 [cited 2025 Oct 5];38(6):1803–9. doi: 10.4067/S0717-95022020000601803
Cortés-Monroy C, Soza S. Una mirada desde la medicina física y rehabilitación al dolor miofascial. Rev Méd Clín Condes [Internet]. 2019 [cited 2025 Oct 1];30(6):428–35. doi: 10.1016/j.rmclc.2019.11.002
Plaut S. Scoping review and interpretation of myofascial pain/fibromyalgia syndrome: An attempt to assemble a medical puzzle. PLoS One [Internet]. 2022 [cited 2025 Oct 5];17(2):e0263087. doi: 10.1371/journal.pone.0263087
Espí-López GV, Fuentes-Aparicio L, Cogollos-de-la-Peña R, Monzani L, Marques-Sule E, Pavlu D, et al. Effects of self-assisted manual therapy combined with a high-intensity walking program on musculoskeletal pain, functionality, and posture in older adults: a multicentre randomized controlled trial. Life (Basel) [Internet]. 2025 [cited 2025 Sep 10];15(6):844. doi: 10.3390/life15060844
Naugle KM, Blythe C, Naugle KE, Keith NC, Riley ZA. Kinesiophobia predicts physical function and physical activity levels in chronic pain-free older adults. Front Pain Res (Lausanne). [Internet]. 2022 [cited 2025 Oct 5];3:874205. doi: 10.3389/fpain.2022.874205
Rethman KK, Mansfield CJ, Moeller J, De Oliveira Silva D, Stephens JA, Di Stasi S, et al. Kinesiophobia is associated with poor function and modifiable through interventions in people with patellofemoral pain: a systematic review with individual participant data correlation meta-analysis. PhysTher [Internet]. 2023 [cited 2025 Oct 5];103(9). doi: 10.1093/ptj/pzad074.